Industries
DigitalOwl is the leading AI-powered platform for insurance and legal industries. We transform complex medical records into structured data for faster, more accurate medical record reviews and enhanced decision-making.






















Speed up medical reviews with concise summaries and automation, freeing up time to focus on critical tasks.

Cut through the noise with quick and accurate medical summaries tailored to your line of business that ensure no detail is missed and that irrelevant and duplicate information is suppressed.

Convert unstructured data into structured data, allowing for machine to machine processing to fully automate the process.

Enhance the accuracy of risk assessments with reliable, AI-enhanced analysis that provides click-to-evidence for easy verification. You are one click away from the truth, ensuring no black box.


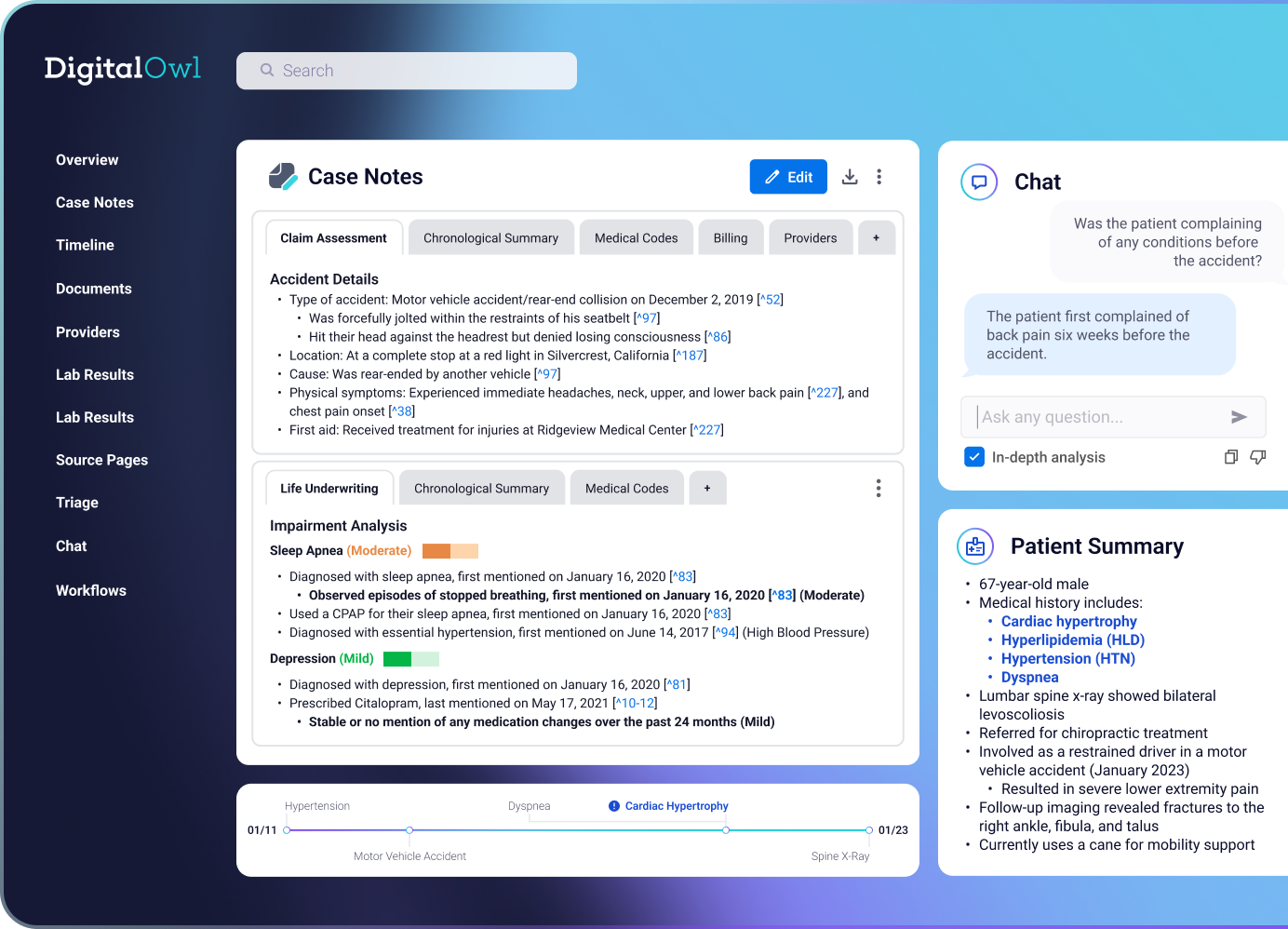
While traditional AI-powered summaries provide considerable value and time efficiency over manual medical record reviews, Case Notes takes these advantages further, offering actionable insights tailored to each line of business. It also enables the analysis and creation of demand packages in relation to the medical data.








































Access quick and accurate medical summaries that surface all relevant information and provide a chronological, 360-degree view of all impairments in one place.
Learn MoreSummarize all vital information, filter for specific impairments and body parts, identify soft medical terms, monitor changes in condition status and chat with medical records to bypass the time-consuming search for details.
Learn MoreMaximize efficiency and reduce costs without overlooking any details amid vast data and pages, filter for critical information and triage cases that fit the claims, pinpointing the crucial information that can make or break a case.
Learn More
